While savouring your favourite chocolate chip ice cream, a sudden jolt of pain runs through your tooth. It’s not just discomforting; it also distracts you from enjoying your favourite food. It makes you wonder if this is an early sign of a cavity forming?
The ugly truth is, tooth decay is far more complicated than being a simple annoyance; it’s a progressive but preventable disease that affects millions every year. But do you ever stop to wonder if tooth decay is caused by unlucky genetics or something that you can actually control? And once the tooth starts decaying, is there any way to stop its spread and save your teeth?
In this blog, we have attempted to answer all these critical questions. The blog helps you recognise, understand, and halt tooth decay irrespective of your background or genetics. If your aim is to deal with your current cavities and avoid getting new ones, then read the full blog for some real, practical solutions to help you tackle tooth decay.
So, Can You Stop Tooth Decay From Spreading?
The short answer is YES. Tooth decay can often be halted or slowed down if caught in time and addressed with the right strategies. While some medical issues resolve naturally, tooth decay can be relentless if the bacteria start to dissolve your enamel. This is a continuous process unless interrupted.
Here are two ways to tackle tooth decay:
- Early decay is often visible as white spots and causes mild sensitivity. It can be reversed by improving oral hygiene and fluoride.
- Active cavities are often visible holes, cause pain and discoloration of the teeth. Individuals often need professional dental care to restore the tooth structure and remove active decay.
Don’t make the mistake of ignoring this problem, as it only accelerates the tissue loss and the treatment becomes more complex and will get costlier over time. Remember that timely action is crucial. Don’t wait for the pain to increase and immediately respond to any changes that you may notice.
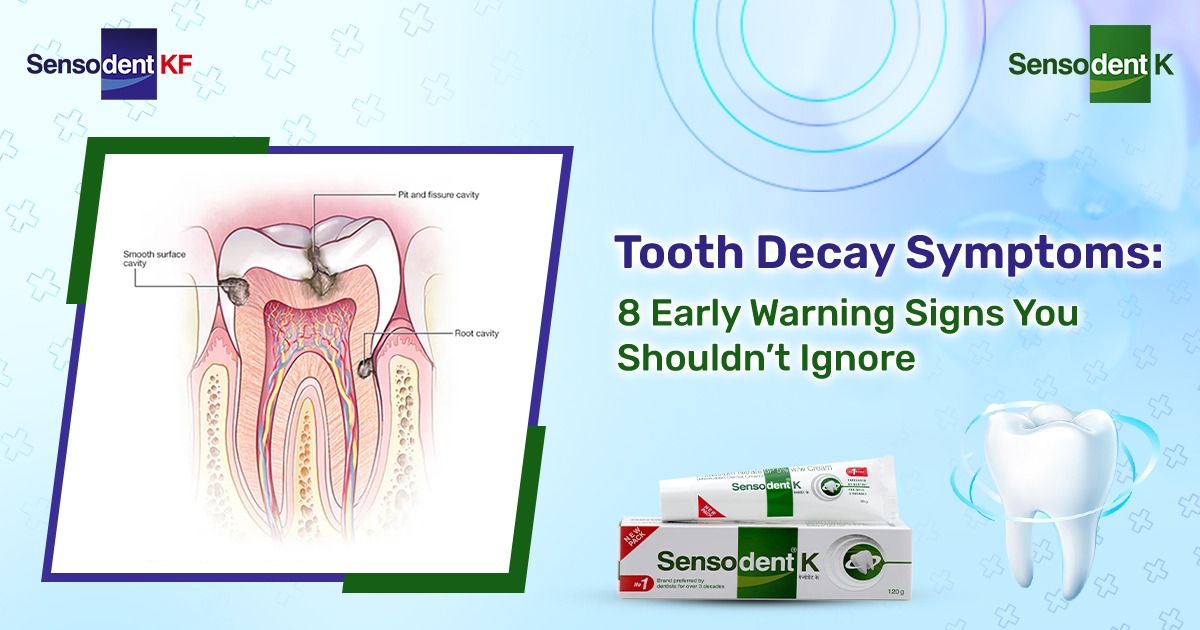
How Does Tooth Decay Progress? What’s The Science of Cavities?
Tooth decay won’t happen overnight. Your teeth will go through clearly defined stages, where every stage offers the opportunity for intervention.
1. Formation of Plaque
Plaque is a sticky biofilm that will build up on your teeth within hours after drinking or eating. Plaque is loaded with bacteria that thrive on sugar, produce acids known as metabolic byproducts.
2. Demineralization and Acid Attack
Whenever you eat something that’s sugary or starchy, the bacteria will feast on it to create acids. These acids begin to leach minerals from your enamel and cause it to lose strength.
3. Breaking Down of the Enamel
Prolonged acid exposure will create tiny pores and weak spots in the enamel, and this will eventually form white spots. This is the first visible sign of demineralization, which gets more severe over time if left untreated.
4. Dentin Exposure
Once the acid erodes the enamel, the softer dentin that’s underneath will be exposed. Dentin will decay rapidly, and it transmits sensitivity to the nerves.
5. Cavity Formation
Tooth decay eventually progresses to form visible pits, holes, or lesions that reach the tooth nerve, leading to infection, abscess, and ultimately resulting in tooth loss.
6. Pulp Damage
The innermost layer of your tooth is called the pulp. It contains the blood and nerve vessels that keep your tooth alive and provide vital sensation. When tooth decay progresses deep enough to reach this layer, the pulp gets irritated and can cause swelling. The hard tooth structure around the pulp can’t expand and leads to intense pressure on the nerves to cause significant pain and sensitivity. Some of the symptoms may include a throbbing pain, especially when chewing or drinking hot/cold liquids.
Getting treatment at this stage requires a root canal. During a root canal, the dentist will remove the infected pulp, clean and seal the tooth. If there’s extensive damage, an extraction may be advised.
7. Abscess
When tooth decay advances into the pulp, bacteria invade to cause severe infection. Increased inflammation in the tooth will lead to a pocket of pus formation at the bottom of your tooth, called an abscess.
Tooth abscesses cause severe pain that may radiate into the jaw. Some of the other symptoms may include swelling of the gums, the face, or jaw, which can cause a fever and cause the lymph nodes in your neck to swell.
Tooth abscesses require prompt treatment as the infection spreads in your jaw bones and other areas of your head and neck. In some cases, the treatment may involve removing the affected tooth.
Key science: Every intervention may remineralize the enamel and reverse white spot lesions. Deeper cavities require restorative treatment.
Is Tooth Decay Hereditary?
A lot of people assume that cavities are a result of inattention or bad oral hygiene, but genetics also plays a surprisingly strong role.
1. Enamel Strength & Structure
Mutations in AMELX and ENAM, along with other enamel-related genes, will produce thinner or less mineralised enamel. A thinner enamel is more prone to acid dissolution, especially if your personal hygiene or diet is less than perfect.
2. Dentin Morphology
Your genetics will influence the number and diameter of the dentin tubules and impact sensitivity and decay. If you’ve inherited porous or weak dentin, the bacteria and acid will have an easier time reaching the tooth nerves, causing pain.
3. Oral Microbiome & Immune Response
Genes shape the balance of “good†and “bad†bacteria in your mouth as well as the saliva’s ability to regulate it. Some people have immune systems that will naturally keep harmful oral bacteria in check. Others are at a higher risk for rapid plaque decay and buildup.
4. Saliva Production & Composition
Attributes like quantity, mineral content, and pH of saliva are genetically dependent. People who naturally produce low saliva (those with conditions like a dry mouth) are at higher risk, as the acids aren't often neutralised as efficiently.
5. Inherited Disorders
People with rare genetic diseases like amelogenesis imperfecta, dentin genesis imperfecta, or enamel hypoplasia directly compromise the tooth structure and can make managing decay a lifelong struggle.
The risk for cavities is high if it’s written in your DNA, but daily habits and professional care will play a more decisive role in preventing tooth decay.
What are the Body’s Natural Defences Against Tooth Decay?
Understanding your natural defences is key to using them to your advantage.
Enamel
The Enamel is the hardest, most resilient tissue in the human body. The enamel is formed by hydroxyapatite crystals. The thickness and integrity (this is often genetically set) will determine how well your teeth will resist acids.
Dentin
This layer exists beneath the enamel and is made of microscopic tubules that will transmit sensation and pain. When the decay reaches your dentin, the sensitivity develops, accelerating decay.
Saliva
Your saliva contains enzymes (such as amylase) and minerals (phosphate, calcium) that work continually to repair and protect your teeth. The saliva also:
- Washes away food particles
- Neutralizes acids after eating food
- Maintains the pH balance in your mouth
Genetic variations that impact enamel strength, saliva composition, and immune response can increase vulnerability to tooth decay. However, targeted oral care and preventive strategies can help offset these inherited risks, allowing individuals to maintain better dental health despite their genetic predisposition.
How Does Your Lifestyle and Environment Cause Tooth Decay?
When it comes to the health of your teeth, daily behaviours will form the foundation of decay prevention and control.
Bad Dietary Habits:
- Acidic drinks like soda, juice, and wine will erode your enamel directly.
- High sugar intake feeds plaque-producing bacteria.
- Frequent snacking means the acids in your mouth linger longer.
Good Dietary Habits:
A mineral-rich diet, like dairy, fish, and green leafy vegetables, supports remineralization.
Brushing and Flossing Techniques
- Aggressively brushing your teeth, using hard-bristle brushes, or skipping flossing allows the plaque to thrive and causes the enamel to wear down.
- An excellent dental routine targets all surfaces, including the teeth and the gumline.
Hydration and Salivary Flow
Alcohol, certain medications, dehydration, and certain medical conditions, such as diabetes, reduce saliva and accelerate the decay process.
Tobacco and Alcohol Use
Chewing tobacco and smoking will increase plaque and tartar, stain the teeth, and reduce saliva. Alcohol is known to dehydrate and cause acid production.
Medical Conditions and Stress
Medical conditions like Sjögren’s syndrome, diabetes, or GRED raise decay risk, cause a dry mouth, and increase acidity.
When it comes to your teeth, what matters than what you eat is how you care for your body and teeth daily.
What are the Early Signs and Symptoms of Tooth Decay
Catching tooth decay early is essential for stopping its spread. Here are some early signs and symptoms to look out for:
Sensitivity to Hot, Cold, or Sweets:
This often indicates thinning of the enamel or exposed dentin, a sign of advancing decay.
White Spots:
Early signs of demineralization will typically appear near the gumline or in the grooves of molars.
Visible Discoloration:
Brown or black spots may signal progressing cavities.
Surface Changes:
Small pits, rough spots, or holes mean decay has breached the enamel.
Persistent Bad Breath or Taste:
- Brush twice daily. Use fluoride toothpaste and a soft-bristle brush. Remember to brush for at least two minutes each time and replace the brush every 3 months.
- Floss at least once a day. It’s critical for cleaning between teeth, where most cavities start.
Decaying tissue and bacterial growth cause ongoing odour or an unpleasant taste.
Don’t ignore mild symptoms as prompt action saves teeth, time, and money.
Comprehensive Strategies That Will Halt Decay
Generally, a multifaceted approach works best as all elements matter. Here are some things you can do:
Consistent Oral Hygiene
Professional Fluoride Use
A prescription-strength fluoride mouthwash or gel can reverse the early signs of decay and fortify the enamel.
Dental office treatments
The varnishes or gels that are administered by dentists are significantly more potent than over-the-counter options available.
Targeted Dietary Changes
Cut sugars and refined starches. Increasing your calcium, phosphate, and vitamin D intake will strengthen your enamel. Chew on sugar-free gum or snacks to boost the production of saliva after meals.
Saliva Support and Dry Mouth Management
To increase the production of saliva, remember to drink water throughout the day. Use artificial saliva products or lozenges for tackling a dry mouth. Avoid alcohol and caffeine, as they both decrease natural saliva.
Sealants and Remineralizing Agents
A dental sealant will protect your vulnerable grooves and pits, especially in children and high-risk adults. Remineralizing toothpaste and powders will help restore enamel minerals.
Timely Intervention
Address your known cavities quickly. Get fillings, crowns, or necessary restorations done. Regular dental cleanings will remove plaque and tartar buildup.
By combining these steps, you create an environment hostile to decay and friendly to lifelong dental health.
Regular Dental Visits and Professional Treatments
Preventive dentistry makes all the difference. Here’s what’s important to remember:
- Biannual checkups help catch problems early. Get advice tailored to your changing needs.
- Professional cleaning will remove built-up tartar and plaque that at-home care can’t address.
- A sealant application will shield hard-to-clean molar pits and prevent new cavities.
- Restorative treatments like fillings, crowns, and root canals save teeth, restore structure, and relieve pain.
- A partnership with your dentist protects against surprises and major interventions.
Managing Hereditary Risk: Personalised Prevention
If “bad teeth†run in your family, don’t despair. Empower yourself with these personalised strategies:
Genetic consultation:
Discuss your family history with your dentist. Ask about genetic markers for enamel or dentin defects.
Custom prevention plans:
Dentists can recommend special products, more frequent cleanings, or targeted fluoride treatments if you’re at high risk.
Awareness and education:
Share risk factors with other family members, encouraging them to take extra steps before decay appears.
Future Innovations: Genetic Testing and Precision Care
Cutting-edge science is reshaping dentistry. Here’s how:
Genetic testing:
Pinpoints your personal risk for cavities, gum disease, and even dry mouth based on DNA markers.
Precision dental care:
The future may bring custom preventive regimens, nutritional plans, and products selected for your unique oral health profile.
AI and digital health tracking:
Smart apps and digital tools will increasingly help you monitor and adjust your habits, automating reminders and optimal care.
Conclusion
Tooth decay can feel overwhelming, but it is preventable and manageable. Science has revealed robust links between genetics, habits, and environmental factors for cavity risk. But with knowledge and discipline, anyone can stop decay from spreading. The foundation lies in:
- Gentle, thorough brushing and flossing
- Fluoride as a daily and professional tool
- Smart dietary choices and hydration
- Attentive management of dry mouth or family risk
- Regular dental visits for monitoring and intervention
Understand your unique risks, invest in disciplined daily care, and trust your dental team to guide ongoing prevention. The earlier you act, the bigger the benefit.
Take Charge: Consult Your Dentist and Try SensodentK
If you’re facing increased cavity risk, whether due to genetics or lifestyle, seeking professional guidance is the first step. Ask your dentist for a personalised plan, consider advanced fluoride treatments, and make routine care a priority.
And, for day-to-day protection, consider Sensodent K Toothpaste. Clinically formulated for sensitive and vulnerable teeth, it strengthens enamel, soothes sensitivity, and offers added defence against decay triggers.