Tooth decay is one of the most widespread oral health problems worldwide, yet many people don’t notice it until discomfort begins. Understanding what it is, why it happens, and how early signs appear can help prevent long-term damage.
What Is Tooth Decay?
Tooth decay begins when bacteria in dental plaque produce acids that gradually weaken and break down the tooth’s outer surface (enamel). If not treated, this process can progress deeper into the tooth and lead to cavities, pain, and infection.
Tooth decay definition
Tooth decay is the gradual destruction of tooth enamel caused by acids produced when bacteria feed on sugars and starches left on your teeth. As minerals are lost, enamel softens, making the tooth more vulnerable to damage. If this mineral loss continues, a cavity (a small hole) can form.
Is tooth decay the same as dental caries?
Yes. The terms “tooth decay†and “dental caries†refer to the same condition. “Dental caries†is the scientific term, while “tooth decay†is commonly used in everyday language. Both describe the breakdown of tooth structure caused by acids produced by bacteria.
How common is tooth decay?
Tooth decay is one of the most common health conditions globally. According to the WHO, untreated dental caries in permanent teeth is the most widespread oral disease, affecting billions worldwide. It occurs in both children and adults and remains highly preventable with good oral hygiene and regular dental care.
Tooth Structure & How Tooth Decay Begins
To understand how decay develops, it helps to know how a healthy tooth is built. Tooth decay doesn’t appear suddenly — it starts with subtle changes on the tooth surface before progressing deeper into the layers.
Enamel, dentin & pulp explained
A tooth has three main layers. Enamel is the hard, outer protective layer and the strongest substance in the human body. Beneath it lies dentin, a softer, porous layer that sends signals to the nerves. At the center is the pulp, which contains nerves and blood vessels that keep the tooth alive. Decay typically starts in the enamel and gradually moves inward toward the pulp.
What is enamel demineralization?
Enamel demineralization is the earliest stage of tooth decay. When bacteria in plaque produce acids, these acids pull away essential minerals like calcium and phosphate from enamel. This weakens the tooth surface and can create white spots — a sign that decay is beginning. At this stage, the process is still reversible with fluoride and good oral hygiene.
Role of saliva in tooth protection
Saliva plays a crucial role in maintaining oral health. It washes away food particles, neutralizes harmful acids, and supplies essential minerals to help enamel repair itself. Low saliva flow — caused by dehydration, medications, or certain medical conditions — increases the risk of tooth decay because the mouth loses its natural defense system.
How plaque forms on teeth
Plaque is a sticky, colorless film of bacteria that constantly forms on teeth. It develops when bacteria feed on sugars and starches left behind after eating or drinking. If plaque isn’t removed through brushing and flossing, it hardens into tartar and continuously produces acids that attack enamel, starting the decay process.
What Causes Tooth Decay?
Tooth decay develops through a gradual process driven by several everyday factors. While bacteria play the main role, your diet, oral hygiene habits, saliva flow, and overall lifestyle all influence how quickly decay progresses. Understanding these causes can help you take steps to stop decay early or prevent it altogether.
- Oral bacteria and acid production
Harmful bacteria in plaque break down sugars and produce acids. These acids continuously attack and weaken tooth enamel. - Sugar & carbohydrate consumption
Frequent intake of sugary or starchy foods feeds bacteria, increasing acid production and speeding up enamel breakdown. - Poor oral hygiene
Irregular brushing and flossing allow plaque to build up, giving bacteria more time to damage the tooth surface. - Acidic foods & beverages
Drinks like soft drinks, fruit juices, and sports drinks soften enamel, making it more vulnerable to decay. - Dry mouth (xerostomia)
Low saliva flow reduces the mouth’s ability to wash away food and neutralize acids, increasing the risk of early decay. - Lack of fluoride
Without enough fluoride from toothpaste, water, or treatments, enamel becomes less resistant to acid attacks. - Genetic factors & enamel strength
Natural variations in enamel hardness or tooth shape can make some people more prone to plaque buildup and decay. - Lifestyle causes (smoking, alcohol)
Smoking reduces saliva flow and affects gum health, while frequent alcohol use can dry the mouth and expose teeth to acids.
Related Blog: What Causes Tooth Decay? 10 Common Risk Factors You Should Know
Stages of Tooth Decay
Tooth decay progresses in clear stages, starting with subtle mineral loss on the tooth surface and advancing deeper into the enamel, dentin, and finally the pulp. Recognizing these stages helps you understand when decay can be reversed—and when professional treatment becomes essential.
Stage 1 – Demineralization (white spots)
The earliest sign of decay is the appearance of white or chalky spots on enamel. At this stage, acids from plaque have begun pulling minerals from the tooth surface. This phase is still reversible with fluoride, improved brushing, and reduced sugar intake.
Stage 2 – Enamel decay
As minerals continue to dissolve, enamel weakens and small cavities may form. You may not feel symptoms yet, but the damage is permanent. A dentist typically treats this stage with a filling to stop the decay from spreading.
Stage 3 – Dentin decay
Once decay reaches the dentin, it progresses more quickly because dentin is softer and more porous. You may begin noticing sensitivity to hot, cold, or sweet foods. Prompt treatment is important to prevent deeper infection.
Stage 4 – Pulp infection
At this stage, bacteria reach the pulp—the inner chamber containing nerves and blood vessels. This can cause persistent toothache, inflammation, and sharp pain. Treatment often involves root canal therapy to remove infected tissue and save the tooth.
Stage 5 – Tooth abscess
If the infection spreads beyond the pulp, an abscess can form at the root tip. This leads to severe pain, swelling, and sometimes fever. An abscess is a dental emergency requiring immediate care to prevent complications.
How fast does tooth decay spread?
The speed of decay varies. Early stages can take months or years depending on diet, hygiene, saliva flow, and fluoride exposure. Once bacteria reach dentin, decay progresses faster due to the layer’s softer structure. Without treatment, advanced stages can develop quickly.
Signs & Symptoms of Tooth Decay
Tooth decay often starts quietly, with many people noticing changes only when the damage has progressed. Paying attention to early signs can help you seek timely care and prevent the decay from reaching deeper layers of the tooth.
Common symptoms include:
- White, brown, or black spots on the tooth surface
- Sensitivity to hot, cold, or sweet foods and drinks
- Toothache or sharp pain, especially when chewing
- Bad breath or an unpleasant taste in the mouth
- Visible holes or pits in the tooth
- Swelling or redness around the affected tooth (in more advanced stages)
Related Blog: Tooth Decay Symptoms: 8 Early Signs You Shouldn’t Ignore
Types of Tooth Decay
Tooth decay can develop in different areas of the mouth, and each type has its own pattern and level of risk. Understanding where decay forms can help you spot early warning signs and know when to seek dental care.
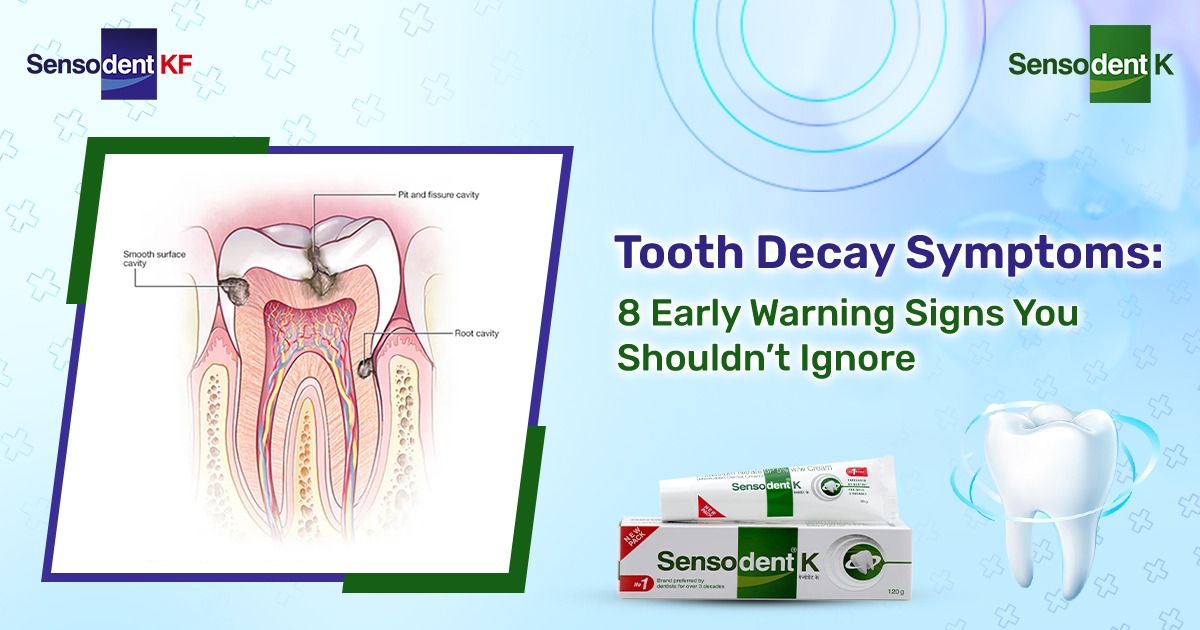
Pit and fissure decay
This type affects the deep grooves on the chewing surfaces of back teeth. These narrow pits and fissures easily trap food and plaque, making them one of the most common sites for cavities—especially in children and teenagers.
Smooth surface decay
Smooth surface decay occurs on the flat, outer surfaces of teeth. It develops slowly and is often preventable with good brushing, flossing, and fluoride. These cavities typically form where plaque accumulates near the gumline.
Root surface decay
When gums recede, the tooth roots become exposed. Since roots are not covered by enamel, they are more vulnerable to decay. Root decay is more common in older adults and those with gum disease or dry mouth.
Recurrent decay
Recurrent or secondary decay forms around the edges of existing fillings, crowns, or dental restorations. Plaque can sneak into tiny gaps or weakened areas, leading to new decay around previously treated teeth.
Baby bottle tooth decay
Also called early childhood caries, this type affects infants and toddlers. It often occurs when a child frequently consumes sugary drinks—such as milk, juice, or formula—especially before sleep, allowing sugars to pool around the teeth.
Tooth Decay by Age Group
Tooth decay affects people at every stage of life, but the risks and patterns change with age. Different age groups face unique challenges based on tooth development, lifestyle habits, and oral health conditions.
Infants and toddlers
Young children are vulnerable to early childhood caries, especially if they consume sugary drinks or milk frequently, including at bedtime. Their enamel is thinner, and brushing depends on adult supervision, increasing the risk of rapid decay.
Children and teenagers
Back teeth with deep grooves make kids and teens prone to pit and fissure cavities. Frequent snacking, sugary drinks, and inconsistent brushing add to the risk. Fluoride use and dental sealants help protect this age group.
Adults
Adults experience decay on both tooth surfaces and around old fillings or crowns. Busy routines, high-carb diets, and irregular dental visits often contribute to cavities forming on smooth surfaces or between teeth.
Older adults
Tooth decay becomes more common with age due to gum recession, which exposes the softer tooth roots. Many older adults also experience dry mouth from medications or medical conditions, reducing saliva protection and increasing decay risk.
How Dentists Diagnose Tooth Decay
Tooth decay isn’t always visible or painful in its early stages, which is why routine dental check-ups are essential. Dentists use a combination of visual examination, tools, and imaging techniques to identify decay before it becomes advanced. Early detection allows for simpler, more effective treatment.
During an appointment, your dentist looks for signs such as discoloration, plaque buildup, or softened enamel. If anything appears suspicious, further tests help confirm the extent of decay and determine the most appropriate treatment. These methods ensure that even hidden or between-tooth cavities are caught early.
Can Tooth Decay Be Reversed?
In its earliest stage, tooth decay can be stopped—and in many cases, reversed. When decay is limited to enamel demineralization, the tooth has not yet developed a cavity, meaning the surface is still intact. At this point, minerals can be restored with the right care.
Reversal is not possible once decay breaks through enamel and forms a hole. From that stage onward, professional treatment is needed. Knowing where your tooth stands helps determine whether at-home care or dental intervention will be effective.
Treatment Options for Tooth Decay
Once a cavity forms, professional treatment is necessary to stop the decay and restore the tooth. Dentists choose the treatment based on how far the decay has progressed, aiming to protect as much natural tooth structure as possible.
Fluoride treatments
Fluoride varnishes or gels help strengthen enamel and can reverse very early decay. These treatments restore lost minerals and make teeth more resistant to acid attacks.
Dental fillings
When decay creates a small to medium-sized cavity, the dentist removes the damaged portion and fills the space with materials like composite resin or amalgam. This restores the tooth’s shape and prevents further spread.
Crowns
For extensive decay that weakens a large area of the tooth, a crown may be needed. A crown covers the entire visible part of the tooth, providing strength and protection.
Root canal treatment
If decay reaches the pulp, a root canal is required to remove infected tissue and relieve pain. The tooth is then sealed and often covered with a crown for added support.
Tooth extraction
Severely damaged teeth that cannot be restored may need to be removed. After extraction, options like implants, bridges, or dentures can replace the missing tooth.
How to Prevent Tooth Decay
Tooth decay is largely preventable with habits that protect enamel and limit bacterial growth. Small changes in daily routines can make a significant difference, especially when combined with regular dental care. Prevention focuses on reducing acid attacks, strengthening teeth, and keeping plaque under control.
Consistent oral hygiene, mindful eating, and the right use of fluoride go a long way in keeping teeth healthy. These steps help stop new decay from forming and prevent existing early-stage decay from progressing.
Tooth Decay & Diet
Diet plays a major role in how quickly decay develops. What you eat, how often you eat it, and how long food stays on your teeth can all influence enamel health. For an Indian audience, where meals often include carbohydrates, sweets, and frequent snacking, mindful choices can significantly reduce the risk of decay.
Here are important diet-related factors to consider:
- Limit frequent sugary foods such as ladoos, pastries, chocolates, and packaged sweets that fuel acid-producing bacteria.
- Reduce sugary drinks like soft drinks, sweetened lassi, fruit juices, and energy drinks, which erode enamel.
- Be cautious with sticky snacks such as jaggery-based chikkis, toffees, or caramel sweets that cling to teeth.
- Balance meals with fibre-rich foods like fruits, vegetables, and whole grains that help clean the mouth naturally.
- Drink more water throughout the day, ideally fluoridated tap water, to wash away food particles and neutralise acids.
- Avoid constant snacking, as frequent eating—especially of namkeen, sweets, or biscuits—keeps acid levels high.
Home Remedies for Tooth Decay
Home remedies cannot cure cavities, but they can support oral health and slow early enamel damage when used alongside good hygiene. These practices help reduce bacteria, strengthen enamel, and maintain a cleaner mouth—especially useful between dental visits.
Here are some helpful, safe home-care practices:
- Brush twice daily with fluoride toothpaste to strengthen enamel and protect against early decay.
- Floss or use interdental cleaners to remove plaque from areas your brush cannot reach.
- Rinse with salt water to reduce bacteria and soothe mild gum irritation.
- Use a fluoride mouthwash, especially if you’re prone to cavities or have early white-spot lesions.
- Chew sugar-free gum, preferably containing xylitol, to boost saliva flow and neutralise acids.
- Stay hydrated, as adequate water intake helps maintain saliva production and natural enamel repair.
Myths & Misconceptions About Tooth Decay
Many people rely on home stories, online advice, or cultural beliefs when it comes to dental care. While some of these tips seem harmless, they often lead to delayed treatment and worsening decay. Clearing up these myths helps you make informed decisions and protect your teeth more effectively.
Common misconceptions include:
- “If there’s no pain, there’s no decay.â€
Early decay is usually painless and can progress quietly until it reaches deeper layers of the tooth. - “Brushing harder cleans better.â€
Aggressive brushing wears down enamel and irritates gums; gentle, thorough brushing is more effective. - “Clove oil can cure cavities.â€
Clove oil may relieve pain temporarily but cannot repair damaged enamel or treat cavities. - “Sugar alone causes tooth decay.â€
Frequency of eating—not just sugar—plays a major role. Frequent snacking keeps acid levels high. - “Only children get cavities.â€
Adults and older adults also face decay, especially around old fillings or exposed tooth roots. - “Traditional remedies can reverse cavities.â€
Remedies may ease discomfort, but only early-stage mineral loss can be reversed—and only with fluoride.
What Happens If Tooth Decay Is Left Untreated?
Ignoring tooth decay allows it to progress from mild enamel damage to deep infection. What starts as small white spots can gradually become cavities, pain, and structural damage. Because decay moves more quickly once it reaches the softer dentin layer, delaying treatment increases the risk of severe complications.
Untreated cavities can lead to persistent pain, difficulty eating, and infections that may spread beyond the tooth. In advanced cases, decay can cause abscesses, tooth loss, and the need for more complex dental procedures. Early treatment helps avoid these issues and preserves both oral health and overall well-being.
How Fluoride-Rich Toothpaste Helps Prevent and Reverse Early Tooth Decay
Fluoride is one of the most effective and scientifically proven ingredients for protecting teeth. When used regularly, fluoride-rich toothpaste strengthens enamel, makes it more resistant to acids, and helps repair early mineral loss. This is why dentists worldwide recommend fluoride products as a core part of daily oral care.
In the earliest stage of decay—when white spots appear—fluoride can actively reverse the damage by restoring minerals to weakened areas of enamel. Even if a cavity has not yet formed, consistent fluoride use can stop the decay from progressing further. For both children and adults, fluoride toothpaste remains a simple, affordable, and essential tool for long-term cavity prevention.
FAQs About Tooth Decay
Tooth decay is a common condition, but many people still have questions about how it develops, how quickly it progresses, and whether it can be reversed. Here are clear answers to some of the most frequently asked questions.
Q1. How fast does tooth decay spread?
Decay usually develops slowly in its early stage and may take months or years to progress through enamel. Once it reaches dentin—the softer layer beneath the enamel—it spreads more quickly. Factors like diet, saliva flow, oral hygiene, and fluoride exposure greatly influence the speed.
Q2. Can tooth decay heal naturally?
Early enamel demineralization can be reversed naturally with help from saliva and fluoride. However, once a cavity forms and a hole appears in the tooth, it cannot heal on its own and will require professional treatment.
Q3. Is tooth decay contagious?
Tooth decay itself is not contagious, but the bacteria that cause decay can be transferred through saliva. Sharing utensils, tasting a child’s food, or close contact can pass cavity-causing bacteria from one person to another.
Q4. Does tooth decay smell?
Yes. Advanced decay can lead to bad breath or an unpleasant taste. This happens when bacteria break down food particles, create acids, or when an infection such as an abscess is present.
Q5. Is tooth decay permanent?
Early stages can be reversed, but once enamel is permanently damaged and a cavity forms, the decay cannot be undone naturally. Treatment such as fillings, crowns, or root canals is needed to restore the tooth.
When Should You See a Dentist?
Tooth decay can progress quietly, so regular dental check-ups are essential even when you have no symptoms. Early detection helps prevent small issues from turning into painful or costly problems. A dentist can identify early enamel changes, remove plaque buildup, and recommend preventive treatments before decay spreads.
You should also schedule a visit if you notice any signs such as sensitivity, toothache, discoloration, or visible holes. Seeking timely care protects your teeth, reduces the risk of infection, and ensures long-term oral health.
Key Takeaways
Tooth decay is common but highly preventable with the right daily habits and timely dental care. Understanding how decay starts and recognizing early signs can help you act before the condition becomes serious. Simple steps like using fluoride toothpaste, reducing sugary foods, and maintaining regular dental visits make a significant difference.
Staying consistent with oral hygiene, paying attention to symptoms, and choosing a tooth-friendly diet can protect your enamel and keep your teeth healthy throughout life.